Thông báo
Vui lòng điền vào thông tin bên dưới
Khẩn cấp
UPPER-GASTROINTESTINAL BLEEDING: CAUSES, EARLY DIAGNOSIS, AND EMERGENCY MANAGEMENT
Upper gastrointestinal bleeding (UGIB) refers to bleeding that occurs in the esophagus, stomach, or duodenum — the upper part of the digestive tract. It is considered a medical emergency because it can lead to rapid blood loss, resulting in hypotension, shock, and potentially death if not diagnosed and treated promptly.
Common Causes
The most common causes of upper gastrointestinal bleeding include:
Peptic ulcer disease: The leading cause, often related to Helicobacter pylori infection or the overuse of nonsteroidal anti-inflammatory drugs (NSAIDs).
Esophageal varices: Common in patients with liver cirrhosis, where increased portal venous pressure causes variceal rupture and massive bleeding.
Mucosal Esophageal Tear – Mallory-Weiss syndrome: Occurs after repeated vomiting.
Severe esophagitis or gastritis: Often due to alcohol, stress, and medications.
Gastric or esophageal cancer: Tumor ulceration leading to bleeding.

Warning Signs
Patients may experience the following:
Vomiting bright red blood or brown material that looks like coffee grounds.
Passing black, tarry stools with a characteristic foul odor.
Signs of blood loss: dizziness, low blood pressure, rapid pulse, sweating, lightheadedness, or even fainting.
These are alarming symptoms that require immediate transfer to the hospital for emergency care. Any delay in treatment can result in a life-threatening situation.

Diagnosis
Doctors typically:
Use a combination of methods to determine the cause and severity of bleeding:
Clinical examination: Assessment of overall condition, blood pressure, pulse, signs of anemia, and degree of shock.
Blood tests: Including complete blood count, coagulation profile, liver and kidney function tests, and electrolytes, to evaluate blood loss and the body’s response capacity.
Upper gastrointestinal endoscopy: The most crucial method, allowing direct visualization of the bleeding site, identification of the cause, and, simultaneously, immediate hemostasis during the endoscopy.
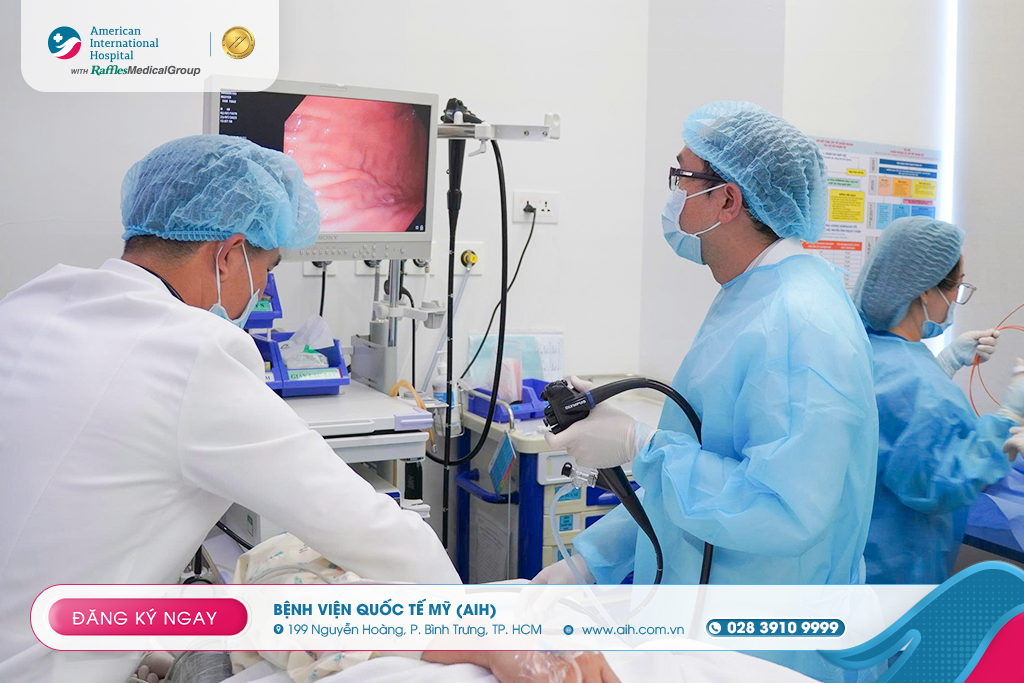
Emergency Management Principles
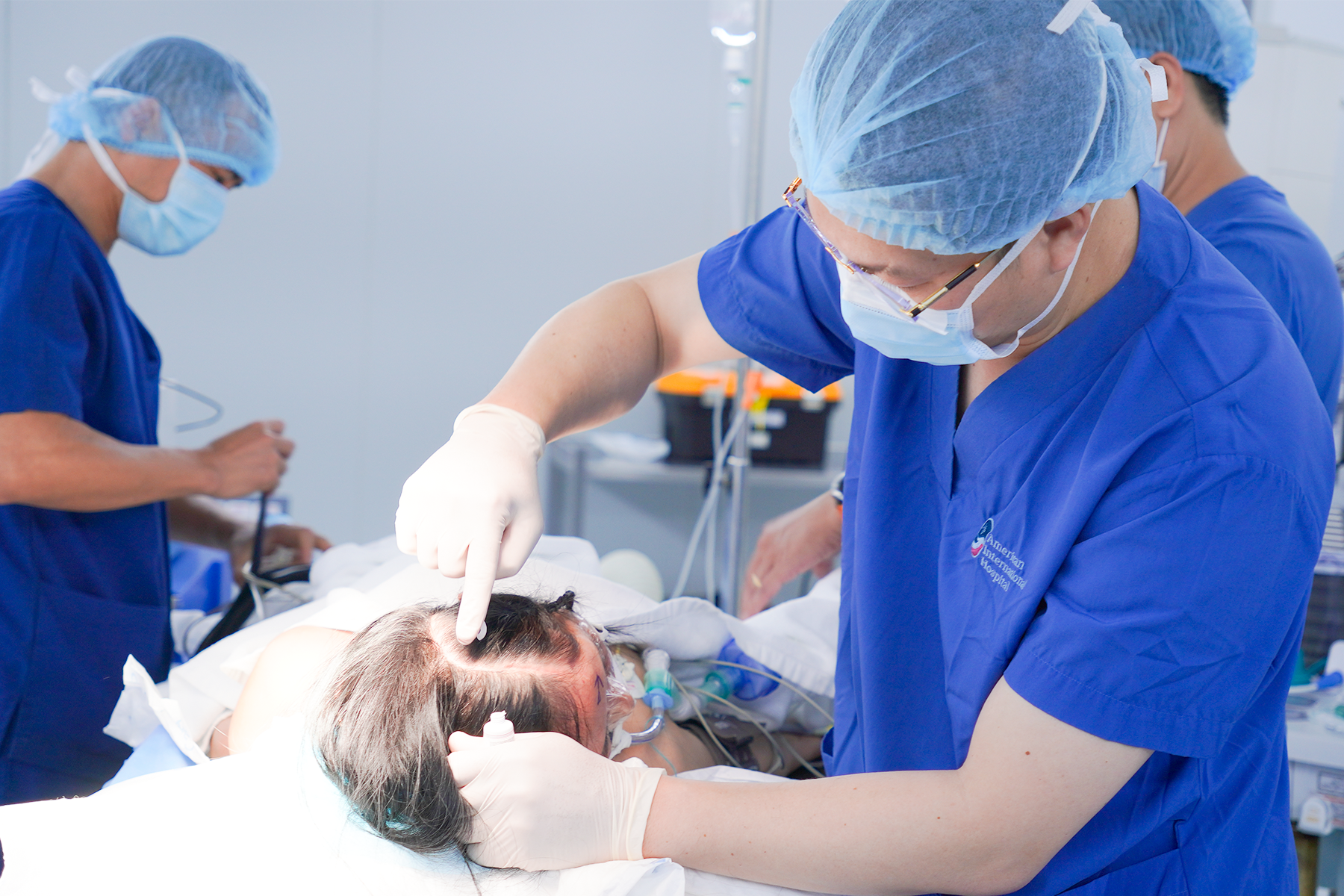
1. Initial Resuscitation:
Establish a large-bore intravenous line to administer fluids or blood transfusions, stabilizing blood pressure and circulating volume.
Monitor pulse, blood pressure, respiratory rate, and urine output.
2. Medical Treatment:
Proton pump inhibitors (PPIs) administered intravenously to reduce acid secretion and promote hemostasis in ulcer-related bleeding.
Vasoconstrictor drugs (e.g., octreotide) in cases of suspected esophageal variceal rupture.
Prophylactic antibiotics for patients with liver cirrhosis.
3. Endoscopic Intervention: Hemostasis can be achieved using clipping, injection therapy, cauterization, or variceal band ligation.
4. Other Interventions: If endoscopic treatment fails, angiographic embolization or surgical intervention may be required.
Post-Emergency Monitoring
Patients should be closely monitored for at least 48–72 hours after emergency treatment to promptly detect any signs of rebleeding.
Alongside emergency care, addressing the underlying cause is crucial:
Eradicate H. pylori infection if peptic ulcer disease is present.
Manage chronic liver disease, reduce portal hypertension, and prevent variceal rebleeding.
Discontinue or replace medications harmful to the stomach or duodenum as advised by the physician.
Prevention of Upper Gastrointestinal Bleeding
Prevention plays a vital role, especially for high-risk individuals:
1. Control Underlying Causes
Treat H. pylori infection thoroughly if diagnosed.
Properly manage chronic liver disease to prevent complications of portal hypertension.
Control chronic conditions such as diabetes, hypertension, and coagulopathies – factors that may exacerbate bleeding severity.
2. Caution in Medication Use
Limit or avoid prolonged use of NSAIDs and corticosteroids.
If such medications are necessary (for bone, joint, or cardiovascular conditions), use gastroprotective agents as prescribed by the doctors.
Do not self-medicate with painkillers, herbal remedies, or unverified dietary supplements.
3. Maintain a Healthy Lifestyle
Avoid alcohol and smoking, both of which damage the gastrointestinal mucosa and liver.
Eat regularly, avoid skipping meals, and limit spicy, greasy, or hard-to-digest foods.
Maintain a healthy weight, as obesity increases the risk of various gastrointestinal disorders.
4. Regular Monitoring and Screening
Individuals with a history of peptic ulcers, gastrointestinal bleeding, or high-risk factors should undergo periodic endoscopic check-ups as recommended.
Patients with liver cirrhosis should be closely monitored, with endoscopic screening for esophageal varices and preventive treatment when necessary.
Upper gastrointestinal bleeding is a serious medical emergency that can be fatal if not managed promptly. However, many cases can be prevented through proper control of underlying conditions, rational medication use, lifestyle modifications, and regular screening. Proactive prevention, combined with early detection and appropriate treatment, is the key to minimizing complications and improving patients’ quality of life.
Reference:
--------------------
Tìm kiếm
Tin tức
Bác sĩ


































































Để lại bình luận